Reproductive System
The major function of the reproductive system is to ensure survival of the species. Other systems in the body, such as the endocrine and urinary systems, work continuously to maintain homeostasis for survival of the individual. An individual may live a long, healthy, and happy life without producing offspring, but if the species is to continue, at least some individuals must produce offspring.
Within the context of producing offspring, the reproductive system has four functions:
o To produce egg and sperm cells
o To transport and sustain these cells
o To nurture the developing offspring
o To produce hormones
These functions are divided between the primary and secondary, or accessory, reproductive organs. The primary reproductive organs, or gonads, consist of the ovaries and testes. These organs are responsible for producing the egg and sperm cells, (gametes), and for producing hormones. These hormones function in the maturation of the reproductive system, the development of sexual characteristics, and have important roles in regulating the normal physiology of the reproductive system. All other organs, ducts, and glands in the reproductive system are considered secondary, or accessory, reproductive organs. These structures transport and sustain the gametes and nurture the developing offspring.
MALE REPRODUCTIVE SYSTEM
All living things reproduce. Reproduction — the process by which organisms make more organisms like themselves — is one of the things that sets living things apart from nonliving things. But even though the reproductive system is essential to keeping a species alive, unlike other body systems it's not essential to keeping an individual alive.
In the human reproductive process, two kinds of sex cells, or gametes, are involved. The male gamete, or sperm, and the female gamete, the egg or ovum, meet in the female's reproductive system to create a new individual. Both the male and female reproductive systems are essential for reproduction.
Humans, like other organisms, pass certain characteristics of themselves to the next generation through their genes, the special carriers of human traits. The genes parents pass along to their offspring are what make kids similar to others in their family, but they're also what make each child unique. These genes come from the father's sperm and the mother's egg, which are produced by the male and female reproductive systems.
Understanding the male reproductive system, what it does, and the problems that can affect it can help you better understand your son's reproductive health.
About the Male Reproductive System
Most species have two sexes: male and female. Each sex has its own unique reproductive system. They are different in shape and structure, but both are specifically designed to produce, nourish, and transport either the egg or sperm.
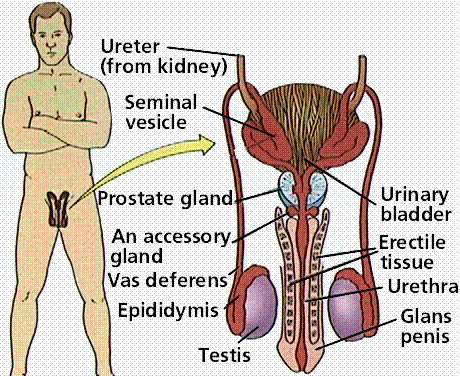
Unlike the female, whose sex organs are located entirely within the pelvis, the male has reproductive organs, or genitals, that are both inside and outside the pelvis. The male genitals include:
• the testicles
• the duct system, which is made up of the epididymis and the vas deferens
• the accessory glands, which include the seminal vesicles and prostate gland
• the penis
In a guy who has reached sexual maturity, the two testicles, or testes, produce and store millions of tiny sperm cells. The testicles are oval-shaped and grow to be about 2 inches (5 centimeters) in length and 1 inch (3 centimeters) in diameter. The testicles are also part of the endocrine system because they produce hormones, including testosterone. Testosterone is a major part of puberty in boys, and as a guy makes his way through puberty, his testicles produce more and more of it. Testosterone is the hormone that causes boys to develop deeper voices, bigger muscles, and body and facial hair, and it also stimulates the production of sperm.
Alongside the testicles are the epididymis and the vas deferens, which make up the duct system of the male reproductive organs. The vas deferens is a muscular tube that passes upward alongside the testicles and transports the sperm-containing fluid called semen. The epididymis is a set of coiled tubes (one for each testicle) that connects to the vas deferens.
The epididymis and the testicles hang in a pouch-like structure outside the pelvis called the scrotum. This bag of skin helps to regulate the temperature of testicles, which need to be kept cooler than body temperature to produce sperm. The scrotum changes size to maintain the right temperature. When the body is cold, the scrotum shrinks and becomes tighter to hold in body heat. When it's warm, the scrotum becomes larger and more floppy to get rid of extra heat. This happens without a guy ever having to think about it. The brain and the nervous system give the scrotum the cue to change size.
The accessory glands, including the seminal vesicles and the prostate gland, provide fluids that lubricate the duct system and nourish the sperm. The seminal vesicles are sac-like structures attached to the vas deferens to the side of the bladder. The prostate gland, which produces some of the parts of semen, surrounds the ejaculatory ducts at the base of the urethra, just below the bladder. The urethra is the channel that carries the semen to the outside of the body through the penis. The urethra is also part of the urinary system because it is also the channel through which urine passes as it leaves the bladder and exits the body.
The penis is actually made up of two parts: the shaft and the glans. The shaft is the main part of the penis and the glans is the tip (sometimes called the head). At the end of the glans is a small slit or opening, which is where semen and urine exit the body through the urethra. The inside of the penis is made of a spongy tissue that can expand and contract.
All boys are born with a foreskin, a fold of skin at the end of the penis covering the glans. Some boys are circumcised, which means that a doctor or clergy member cuts away the foreskin. Circumcision is usually performed during a baby boy's first few days of life. Although circumcision is not medically necessary, parents who choose to have their children circumcised often do so based on religious beliefs, concerns about hygiene, or cultural or social reasons. Boys who have circumcised penises and those who don't are no different: All penises work and feel the same, regardless of whether the foreskin has been removed.
What the Male Reproductive System Does
The male sex organs work together to produce and release semen into the reproductive system of the female during sexual intercourse. The male reproductive system also produces sex hormones, which help a boy develop into a sexually mature man during puberty.
When a baby boy is born, he has all the parts of his reproductive system in place, but it isn't until puberty that he is able to reproduce. When puberty begins, usually between the ages of 10 and 14, the pituitary gland — which is located near the brain — secretes hormones that stimulate the testicles to produce testosterone. The production of testosterone brings about many physical changes. Although the timing of these changes is different for every guy, the stages of puberty generally follow a set sequence.
• During the first stage of male puberty, the scrotum and testes grow larger.
• Next, the penis becomes longer, and the seminal vesicles and prostate gland grow.
• Hair begins to appear in the pubic area and later it grows on the face and underarms. During this time, a male's voice also deepens.
• Boys also undergo a growth spurt during puberty as they reach their adult height and weight.
A male who has reached puberty will produce millions of sperm cells every day. Each sperm is extremely small: only 1/600 of an inch (0.05 millimeters long). Sperm develop in the testicles within a system of tiny tubes called the seminiferous tubules. At birth, these tubules contain simple round cells, but during puberty, testosterone and other hormones cause these cells to transform into sperm cells. The cells divide and change until they have a head and short tail, like tadpoles. The head contains genetic material (genes). The sperm use their tails to push themselves into the epididymis, where they complete their development. It takes sperm about 4 to 6 weeks to travel through the epididymis.
The sperm then move to the vas deferens, or sperm duct. The seminal vesicles and prostate gland produce a whitish fluid called seminal fluid, which mixes with sperm to form semen when a male is sexually stimulated. The penis, which usually hangs limp, becomes hard when a male is sexually excited. Tissues in the penis fill with blood and it becomes stiff and erect (an erection). The rigidity of the erect penis makes it easier to insert into the female's vagina during sexual intercourse. When the erect penis is stimulated, muscles around the reproductive organs contract and force the semen through the duct system and urethra. Semen is pushed out of the male's body through his urethra — this process is called ejaculation. Each time a guy ejaculates, it can contain up to 500 million sperm.
When the male ejaculates during intercourse, semen is deposited into the female's vagina. From the vagina the sperm make their way up through the cervix and move through the uterus with help from uterine contractions. If a mature egg is in one of the female's fallopian tubes, a single sperm may penetrate it, and fertilization, or conception, occurs.
This fertilized egg is now called a zygote and contains 46 chromosomes — half from the egg and half from the sperm. The genetic material from the male and female has combined so that a new individual can be created. The zygote divides again and again as it grows in the female's uterus, maturing over the course of the pregnancy into an embryo, a fetus, and finally a newborn baby.
Things That Can Go Wrong With the Male Reproductive System
Boys may sometimes experience reproductive system problems, including:
Disorders of the Scrotum, Testicles, or Epididymis
Conditions affecting the scrotal contents may involve the testicles, epididymis, or the scrotum itself.
• Testicular trauma. Even a mild injury to the testicles can cause severe pain, bruising, or swelling. Most testicular injuries occur when the testicles are struck, hit, kicked, or crushed, usually during sports or due to other trauma. Testicular torsion, when one of the testicles twists around, cutting off its blood supply, is also a problem that some teen males experience, although it's not common. Surgery is needed to untwist the cord and save the testicle.
• Varicocele. This is a varicose vein (an abnormally swollen vein) in the network of veins that run from the testicles. Varicoceles commonly develop while a boy is going through puberty. A varicocele is usually not harmful, although it can damage the testicle or decrease sperm production. Take your son to see his doctor if he is concerned about changes in his testicles.
• Testicular cancer. This is one of the most common cancers in men younger than 40. It occurs when cells in the testicle divide abnormally and form a tumor. Testicular cancer can spread to other parts of the body, but if it's detected early, the cure rate is excellent. Teen boys should be encouraged to learn to perform testicular self-examinations.
• Epididymitis is inflammation of the epididymis, the coiled tubes that connect the testes with the vas deferens. It is usually caused by an infection, such as the sexually transmitted disease chlamydia, and results in pain and swelling next to one of the testicles.
• Hydrocele. A hydrocele occurs when fluid collects in the membranes surrounding the testes. Hydroceles may cause swelling in the scrotum around the testicle but are generally painless. In some cases, surgery may be needed to correct the condition.
• Inguinal hernia. When a portion of the intestines pushes through an abnormal opening or weakening of the abdominal wall and into the groin or scrotum, it is known as an inguinal hernia. The hernia may look like a bulge or swelling in the groin area. It can be corrected with surgery.
Disorders of the Penis
Disorders affecting the penis include:
• Inflammation of the penis. Symptoms of penile inflammation include redness, itching, swelling, and pain. Balanitis occurs when the glans (the head of the penis) becomes inflamed. Posthitis is foreskin inflammation, which is usually due to a yeast or bacterial infection.
• Hypospadias. This is a disorder in which the urethra opens on the underside of the penis, not at the tip.
• Phimosis. This is a tightness of the foreskin of the penis and is common in newborns and young children. It usually resolves itself without treatment. If it interferes with urination, circumcision (removal of the foreskin) may be recommended.
• Paraphimosis. This may develop when a boy's uncircumcised penis is retracted but doesn't return to the unretracted position. As a result, blood flow to the head of the penis may be impaired, and your son may experience pain and swelling. A doctor may use lubricant to make a small incision so the foreskin can be pulled forward. If that doesn't work, circumcision may be recommended.
• Ambiguous genitalia. This occurs when a child is born with genitals that aren't clearly male or female. In most boys born with this disorder, the penis may be very small or nonexistent, but testicular tissue is present. In a small number of cases, the child may have both testicular and ovarian tissue.
• Micropenis. This is a disorder in which the penis, although normally formed, is well below the average size, as determined by standard measurements.
If your son has symptoms of a problem with his reproductive system or he has questions about growth and sexual development, talk with your doctor — many problems with the male reproductive system can be treated.
FEMALE REPRODUCTIVE SYSTEM
All living things reproduce. Reproduction — the process by which organisms make more organisms like themselves — is one of the things that sets living things apart from nonliving matter. But even though the reproductive system is essential to keeping a species alive, unlike other body systems, it's not essential to keeping an individual alive.
In the human reproductive process, 2 kinds of sex cells, or gametes, are involved. The male gamete, or sperm, and the female gamete, the egg or ovum, meet in the female's reproductive system to create a new individual.
Both the male and female reproductive systems are essential for reproduction. The female needs a male to fertilize her egg, even though it is she who carries offspring through pregnancy and childbirth.
Humans, like other organisms, pass certain characteristics of themselves to the next generation through their genes, the special carriers of human traits. The genes that parents pass along to their children are what make children similar to others in their family, but they are also what make each child unique. These genes come from the male's sperm and the female's egg, which are produced by the male and female reproductive systems.
About the Female Reproductive System
Most species have two sexes: male and female. Each sex has its own unique reproductive system. They are different in shape and structure, but both are specifically designed to produce, nourish, and transport either the egg or sperm.
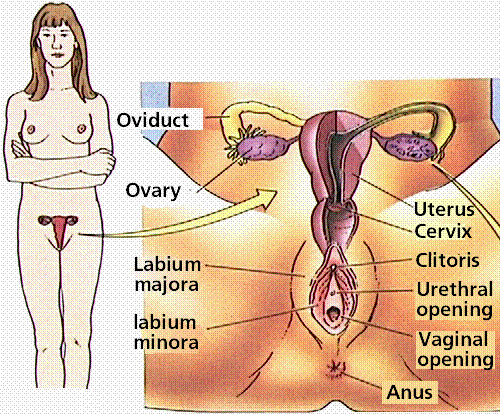
Unlike the male, the human female has a reproductive system located entirely in the pelvis. The external part of the female reproductive organs is called the vulva, which means covering. Located between the legs, the vulva covers the opening to the vagina and other reproductive organs located inside the body.
The fleshy area located just above the top of the vaginal opening is called the mons pubis. Two pairs of skin flaps called the labia (which means lips) surround the vaginal opening. The clitoris, a small sensory organ, is located toward the front of the vulva where the folds of the labia join. Between the labia are openings to the urethra (the canal that carries urine from the bladder to the outside of the body) and vagina. Once girls become sexually mature, the outer labia and the mons pubis are covered by pubic hair.
A female's internal reproductive organs are the vagina, uterus, fallopian tubes, and ovaries.
The vagina is a muscular, hollow tube that extends from the vaginal opening to the uterus. The vagina is about 3 to 5 inches (8 to 12 centimeters) long in a grown woman. Because it has muscular walls, it can expand and contract. This ability to become wider or narrower allows the vagina to accommodate something as slim as a tampon and as wide as a baby. The vagina's muscular walls are lined with mucous membranes, which keep it protected and moist.
The vagina serves three purposes:
1. It's where the penis is inserted during sexual intercourse.
2. It's the pathway that a baby takes out of a woman's body during childbirth, called the birth canal.
3. It provides the route for the menstrual blood (the period) to leave the body from the uterus.
A thin sheet of tissue with one or more holes in it called the hymen partially covers the opening of the vagina. Hymens are often different from female to female. Most women find their hymens have stretched or torn after their first sexual experience, and the hymen may bleed a little (this usually causes little, if any, pain). Some women who have had sex don't have much of a change in their hymens, though.
The vagina connects with the uterus, or womb, at the cervix (which means neck). The cervix has strong, thick walls. The opening of the cervix is very small (no wider than a straw), which is why a tampon can never get lost inside a girl's body. During childbirth, the cervix can expand to allow a baby to pass.
The uterus is shaped like an upside-down pear, with a thick lining and muscular walls — in fact, the uterus contains some of the strongest muscles in the female body. These muscles are able to expand and contract to accommodate a growing fetus and then help push the baby out during labor. When a woman isn't pregnant, the uterus is only about 3 inches (7.5 centimeters) long and 2 inches (5 centimeters) wide.
At the upper corners of the uterus, the fallopian tubes connect the uterus to the ovaries. The ovaries are two oval-shaped organs that lie to the upper right and left of the uterus. They produce, store, and release eggs into the fallopian tubes in the process called ovulation. Each ovary measures about 1½ to 2 inches (4 to 5 centimeters) in a grown woman.
There are two fallopian tubes, each attached to a side of the uterus. The fallopian tubes are about 4 inches (10 centimeters) long and about as wide as a piece of spaghetti. Within each tube is a tiny passageway no wider than a sewing needle. At the other end of each fallopian tube is a fringed area that looks like a funnel. This fringed area wraps around the ovary but doesn't completely attach to it. When an egg pops out of an ovary, it enters the fallopian tube. Once the egg is in the fallopian tube, tiny hairs in the tube's lining help push it down the narrow passageway toward the uterus.
The ovaries are also part of the endocrine system because they produce female sex hormones such as estrogen and progesterone.
What the Female Reproductive System Does
The female reproductive system enables a woman to:
• produce eggs (ova)
• have sexual intercourse
• protect and nourish the fertilized egg until it is fully developed
• give birth
Sexual reproduction couldn't happen without the sexual organs called the gonads. Although most people think of the gonads as the male testicles, both sexes actually have gonads: In females the gonads are the ovaries. The female gonads produce female gametes (eggs); the male gonads produce male gametes (sperm). After an egg is fertilized by the sperm, the fertilized egg is called the zygote.
When a baby girl is born, her ovaries contain hundreds of thousands of eggs, which remain inactive until puberty begins. At puberty, the pituitary gland, located in the central part of the brain, starts making hormones that stimulate the ovaries to produce female sex hormones, including estrogen. The secretion of these hormones causes a girl to develop into a sexually mature woman.
Toward the end of puberty, girls begin to release eggs as part of a monthly period called the menstrual cycle. Approximately once a month, during ovulation, an ovary sends a tiny egg into one of the fallopian tubes.
Unless the egg is fertilized by a sperm while in the fallopian tube, the egg dries up and leaves the body about 2 weeks later through the uterus — this is menstruation. Blood and tissues from the inner lining of the uterus combine to form the menstrual flow, which in most girls lasts from 3 to 5 days. A girl's first period is called menarche.
It's common for women and girls to experience some discomfort in the days leading to their periods. Premenstrual syndrome (PMS) includes both physical and emotional symptoms that many girls and women get right before their periods, such as acne, bloating, fatigue, backaches, sore breasts, headaches, constipation, diarrhea, food cravings, depression, irritability, or difficulty concentrating or handling stress. PMS is usually at its worst during the 7 days before a girl's period starts and disappears once it begins.
Many girls also experience abdominal cramps during the first few days of their periods caused by prostaglandins, chemicals in the body that make the smooth muscle in the uterus contract. These involuntary contractions can be either dull or sharp and intense.
It can take up to 2 years from menarche for a girl's body to develop a regular menstrual cycle. During that time, her body is adjusting to the hormones puberty brings. On average, the monthly cycle for an adult woman is 28 days, but the range is from 23 to 35 days.
If a female and male have sex within several days of the female's ovulation, fertilization can occur. When the male ejaculates (when semen leaves a male's penis), between 0.05 and 0.2 fluid ounces (1.5 to 6.0 milliliters) of semen is deposited into the vagina. Between 75 and 900 million sperm are in this small amount of semen, and they "swim" up from the vagina through the cervix and uterus to meet the egg in the fallopian tube. It takes only one sperm to fertilize the egg.
About a week after the sperm fertilizes the egg, the fertilized egg (zygote) has become a multicelled blastocyst. A blastocyst is about the size of a pinhead, and it's a hollow ball of cells with fluid inside. The blastocyst burrows itself into the lining of the uterus, called the endometrium. The hormone estrogen causes the endometrium to become thick and rich with blood.
Progesterone, another hormone released by the ovaries, keeps the endometrium thick with blood so that the blastocyst can attach to the uterus and absorb nutrients from it. This process is called implantation.
As cells from the blastocyst take in nourishment, another stage of development, the embryonic stage, begins. The inner cells form a flattened circular shape called the embryonic disk, which will develop into a baby. The outer cells become thin membranes that form around the baby. The cells multiply thousands of times and move to new positions to eventually become the embryo.
After approximately 8 weeks, the embryo is about the size of an adult's thumb, but almost all of its parts — the brain and nerves, the heart and blood, the stomach and intestines, and the muscles and skin — have formed.
During the fetal stage, which lasts from 9 weeks after fertilization to birth, development continues as cells multiply, move, and change. The fetus floats in amniotic fluid inside the amniotic sac. The fetus receives oxygen and nourishment from the mother's blood via the placenta, a disk-like structure that sticks to the inner lining of the uterus and connects to the fetus via the umbilical cord. The amniotic fluid and membrane cushion the fetus against bumps and jolts to the mother's body.
Pregnancy lasts an average of 280 days — about 9 months. When the baby is ready for birth, its head presses on the cervix, which begins to relax and widen to get ready for the baby to pass into and through the vagina. The mucus that has formed a plug in the cervix loosens, and with amniotic fluid, comes out through the vagina when the mother's water breaks.
When the contractions of labor begin, the walls of the uterus contract as they are stimulated by the pituitary hormone oxytocin. The contractions cause the cervix to widen and begin to open. After several hours of this widening, the cervix is dilated (opened) enough for the baby to come through. The baby is pushed out of the uterus, through the cervix, and along the birth canal. The baby's head usually comes first; the umbilical cord comes out with the baby and is cut after the baby is delivered.
The last stage of the birth process involves the delivery of the placenta, which is now called the afterbirth. After it has separated from the inner lining of the uterus, contractions of the uterus push it out, along with its membranes and fluids.
Problems of the Female Reproductive System
Your daughter may sometimes experience reproductive system problems. Below are some examples of disorders that affect the female reproductive system.
Problems of the Vulva and Vagina
• Vulvovaginitis is an inflammation of the vulva and vagina. It may be caused by irritating substances (such as laundry soaps or bubble baths). Poor personal hygiene (such as wiping from back to front after a bowel movement) may also cause this problem. Symptoms include redness and itching in the vaginal and vulvar areas and sometimes vaginal discharge. Vulvovaginitis can also be caused by an overgrowth of Candida, a fungus normally present in the vagina.
• Nonmenstrual vaginal bleeding is most commonly due to the presence of a vaginal foreign body, often wadded-up toilet paper. It may also be due to urethral prolapse, a condition in which the mucous membranes of the urethra protrude into the vagina and form a tiny, doughnut-shaped mass of tissue that bleeds easily. It can also be due to a straddle injury (such as when falling onto a beam or bicycle frame) or vaginal trauma from sexual abuse.
• Labial adhesions, the sticking together or adherence of the labia in the midline, usually appear in infants and young girls. Although there are usually no symptoms associated with this condition, labial adhesions can lead to an increased risk of urinary tract infection. Sometimes topical estrogen cream is used to help separate the labia.
Problems of the Ovaries and Fallopian Tubes
• Ectopic pregnancy occurs when a fertilized egg, or zygote, doesn't travel into the uterus, but instead grows rapidly in the fallopian tube. A woman with this condition can develop severe abdominal pain and should see a doctor because surgery may be necessary.
• Endometriosis occurs when tissue normally found only in the uterus starts to grow outside the uterus — in the ovaries, fallopian tubes, or other parts of the pelvic cavity. It can cause abnormal bleeding, painful periods, and general pelvic pain.
• Ovarian tumors, although they're rare, can occur. Girls with ovarian tumors may have abdominal pain and masses that can be felt in the abdomen. Surgery may be needed to remove the tumor.
• Ovarian cysts are noncancerous sacs filled with fluid or semisolid material. Although they are common and generally harmless, they can become a problem if they grow very large. Large cysts may push on surrounding organs, causing abdominal pain. In most cases, cysts will disappear on their own and treatment is unnecessary. If the cysts are painful, a doctor may prescribe birth control pills to alter their growth, or they may be removed by a surgeon.
• Polycystic ovary syndrome is a hormone disorder in which too many male hormones (androgens) are produced by the ovaries. This condition causes the ovaries to become enlarged and develop many fluid-filled sacs, or cysts. It often first appears during the teen years. Depending on the type and severity of the condition, it may be treated with drugs to regulate hormone balance and menstruation.
• Ovarian torsion, or the twisting of the ovary, can occur when an ovary becomes twisted because of a disease or a developmental abnormality. The torsion blocks blood from flowing through the blood vessels that supply and nourish the ovaries. The most common symptom is lower abdominal pain. Surgery is usually necessary to correct it.
Menstrual Problems
A variety of menstrual problems can affect girls, including:
• Dysmenorrhea is when a girl has painful periods.
• Menorrhagia is when a girl has a very heavy periods with excess bleeding.
• Oligomenorrhea is when a girl misses or has infrequent periods, even though she's been menstruating for a while and isn't pregnant.
• Amenorrhea is when a girl has not started her period by the time she is 16 years old or 3 years after starting puberty, has not developed signs of puberty by age 14, or has had normal periods but has stopped menstruating for some reason other than pregnancy.
Infections of the Female Reproductive System
• Sexually Transmitted Diseases, These include infections and diseases such as pelvic inflammatory disease (PID), human immunodeficiency virus/acquired immunodeficiency syndrome (HIV/AIDS), human papillomavirus (HPV, or genital warts), syphilis, chlamydia, gonorrhea, and genital herpes. Most are spread from one person to another by sexual contact.
• Toxic Shock Syndrome, This uncommon illness is caused by toxins released into the body during a type of bacterial infection that is more likely to develop if a tampon is left in too long. It can produce high fever, diarrhea, vomiting, and shock.
If you think your daughter may have symptoms of a problem with her reproductive system or if you have questions about her growth and development, talk to your doctor — many problems with the female reproductive system can be treated
